Movement as Medicine

It is well-accepted that our modern sedentary lifestyle is a huge contributing factor to musculoskeletal problems and cardiorespiratory disease (Manson et al 2004). It is therefore not a giant leap to suggest that the antidote to a lack of movement is more movement. This may sound over-simplistic, because it is. The problem is that it is not easy, and for the most part, people look for the easy solution, such as popping a pill or going to a chiropractor twice a week. It is tempting to hand our problems over to someone else and say “fix me,” but long term this is not an effective strategy. Movement and training work like vaccines and ideally we should be using these as preventative measures against disease. However, it also works very well in treating disease and injury.
To ensure health and longevity we need resilient bodies. Environmental stresses are much greater today than ever before, and the approaches we take need to reflect this. When we think of movement, the systems we primarily mean to train are the cardiovascular, the respiratory, the muscular and the skeletal systems; though training these systems also positively influences all other systems of the body.
The cardiorespiratory system seems to get a lot more love than the musculoskeletal system. Again, I think this is due in part to the relative simplicity of adequately training it. Walking, running, biking, swimming or hiking will generally take care of the health benefits associated with training the cardiorespiratory system.
While keeping your heart healthy with some aerobic exercise is a positive step, it should not be the only step. We need to train our musculoskeletal system with some form of resistance training for optimum health and longevity (Winett and Carpinelli, 2002). We do not need the flexibility of a ballerina, the strength of a powerlifter, the endurance of a marathon runner or the size of a bodybuilder, so we need not train to these extremes. However, we do need to balance our modern lifestyle with intelligent strength training. For many the thought of lifting weights conjures up images of bodybuilders and other negative connotations, so as an industry we need to educate the masses as to what strength training is about, and what it can do for them.
A high percentage of chronic and acute musculoskeletal pain/injuries are attributed to a lack of muscle strength/endurance/flexibility or mobility of the joints, and oftentimes it is a combination of all the aforementioned. As I’ve mentioned, we are a ”use it or lose it” system. We are getting further confirmation of this fact with recent advances in the study of neuroplasticity. It’s important to remember, however, that just as we can lose an ability, we can also regain it through proper training.
Let’s look at low back pain as an example, as it is one of if not the biggest contributor to disability in the industrialised world (Vos, Theo et al 2013). Although no two spines are identical, there are a lot of commonalities between those that suffer from chronic low back pain. Dr. Vladimir Janda’s upper and lower crossed syndrome classifications are an example of this. We know that pain alters motor control, and although this initial mechanism may be protective, it often leads to compensatory movement patterns long after the acute stage. These altered movement patterns lead to altered muscle function, i.e. muscle inhibition or over-activation. These muscle imbalances in turn set us up for chronic problems such as joint degeneration (Janda 1987, 1988).
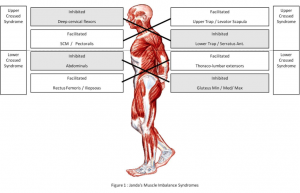
Below we have examples of lower and upper crossed syndrome compared to a more neutral posture:


So what can we do? Post-injury there often needs to be movement re-patterning. Once again using back pain as the example, we need to re-train the body to effectively hinge at the hips to spare the spine (Liebenson 1996). Although it may be complementary, no amount of massage or chiropractic adjustments will help to regain this skill. We need to practice it through movement training. When adequate motor learning has taken place we can add load to the pattern with exercises like deadlifts and begin training fitness and functional tolerance. Back pain is rarely an easy or short term fix as it is a multi-faceted problem, but movement is undoubtedly an essential part of successful recovery.
Summary
We not only need to train the cardiorespiratory system but also the musculoskeletal system for optimal health and longevity. The methods that work in rehabilitation usually work even better in pre-habilitation, preventing the onset of painful dysfunctions.
Closing thoughts
In my opinion, fitness professionals are among the few professions in “health care;” doctors, chiropractors, physios, osteopaths, surgeons etc. are all in what I would call “sick care.” There must be a paradigm shift away from sick care towards preventative medicine such as quality movement practice along with supportive nutrition strategies. It also needs to become a bigger part in the treatment of disease and various musculoskeletal problems.
This blog was written by Ed O’Donovan
Works Cited:
JoAnn E. Manson, MD,DrPH; Patrick J. Skerrett, MS; Philip Greenland, MD; Theodore B. VanItallie, MD The Escalating Pandemics of Obesity and Sedentary Lifestyle. Arch Intern Med. 2004;164(3):249-258.
Richard A. Winett, Ph.Da, 2, Ralph N. Carpinelli, Ed.D.b Potential Health-Related Benefits of Resistance Training.
Global, national and regional incidence, prevalence and years lived with disability for 301 acute and chronic diseases and injuries in 188 countries, 1990-2013: A systematic anaylsis for the global burden of disease project 2013. Vos, Theo et al. THE LANCET.
Assessment and Treatment of Muscle Imbalance: The Janda Approach. Dr. Vladimir Janda 1987 1988.
Rehabilitation of the Spine: A Practitioner’s Manual. Dr Craig Liebenson.